For decades, obstructive sleep apnea (OSA) was wrongly perceived as a condition affecting mostly overweight, older men. Now, research shows that OSA is significantly underdiagnosed in women, especially those entering perimenopause and menopause. By 2050, projections indicate nearly 77 million US adults aged 30-69 will have OSA, with a 65% relative increase in female prevalence compared to just a 19% increase in men. This is not merely an aging or obesity problem; it’s a systemic failure to recognize and treat the condition in half the population.
The Biological Shift: Why Women Are Overlooked
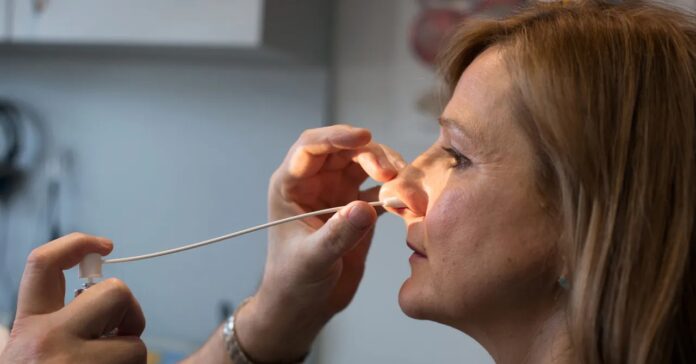
OSA occurs when the upper airway collapses during sleep, causing oxygen levels to drop. While this affects anyone, hormonal changes during menopause dramatically increase a woman’s risk. Estrogen and progesterone provide protection by regulating breathing and maintaining airway muscle tone. As these hormones decline, fat distribution shifts towards the neck, further constricting the airway. This creates a “double whammy,” as described by NYU Grossman School of Medicine’s Rashmi Nisha Aurora: diminishing hormonal defenses combined with increased physical strain.
The issue isn’t just biology; it’s also how OSA presents in women. Symptoms differ from the classic male profile of loud snoring and daytime sleepiness. Women often experience insomnia, mood changes, headaches, or restless sleep—symptoms easily dismissed as menopause itself.
Diagnostic Blind Spots: Tools Designed for Men
Current diagnostic tools are biased towards male symptom expression. The checklists used by doctors, like the Epworth Sleepiness Scale, weren’t validated in women across age groups. This means that many women with OSA don’t fit the traditional diagnostic criteria, and their condition goes undetected.
Women may stop breathing dozens of times an hour without making much noise, making it harder to identify. As ResMed’s Carlos Nunez points out, “Most people don’t realize they have it, because you’re asleep when it happens.” This leads to misdiagnosis, with women often treated for insomnia, anxiety, or even depression instead of addressing the underlying OSA.
Beyond Snoring: The Severity of Undiagnosed OSA
Even “mild” apnea (15 breathing disruptions per hour) can cause significant harm. These frequent oxygen drops lead to vascular injury, metabolic dysfunction, and a higher risk of heart disease. Untreated OSA is increasingly linked to cognitive decline and Alzheimer’s.
The good news is treatment (CPAP) is effective, but even this may differ by sex. Preliminary research suggests women respond differently to CPAP therapy, hinting at the need for personalized approaches. Devices are evolving, with algorithms adjusting pressure dynamically based on individual needs.
The Path Forward: Awareness and Inclusive Research
The most critical step is cultural change. Healthcare systems have historically prioritized male physiology, leaving women understudied. Aurora emphasizes that “we need to be studied because we are complicated.” More inclusive clinical trials are essential, along with better patient and provider education.
The message is clear: if you’re a woman experiencing sleep disturbances, don’t assume it’s just menopause or stress. Demand a thorough evaluation for OSA. The cost of inaction is too high, not just for individual health but for public health as a whole.